Prior to the development of MRI it was difficult to diagnose a tethered cord without utilization of invasive diagnostic procedures. Therefore, many infants were untreated, and it was possible to observe the "natural history" of the untreated tether. It has been a common observation that the majority of these children experience neurological deterioration during childhood or adolescence. Occasionally, sudden and catastrophic neurologic deterioration was associated with normal sports activities or minor injuries. Even the occasional normal child who reaches adulthood is at risk for deterioration in later years. Childbirth may be associated with "precipitous" neurological decline as a result of normal obstetric positioning. It therefore seems clear that the hazard of deterioration is very significant and surgery must always be considered prior to the evolution of neurological decline.
It is always best to carry out surgery for any potential neurological problem before there is evolving symptomatology. In the asymptomatic neonate, the most vulnerable neurological function is bowel and bladder. Obviously, in the neonate, this is difficult to assess, and it is always possible that there may be impairment in either of these functions that is not clinically obvious. In addition, it is well recognized that once bowel and bladder dysfunction evolve, it is difficult to reverse even with technically satisfactory surgery. For this reason, it is the perspective of most pediatric neurosurgeons that all children with a tethered cord must undergo surgery, and it is important that it be carried out before there are neurological symptoms. It has been a general policy to operate sometime between 2 and 4 months of age. In other words, the operation should be performed almost as soon as the diagnosis is made and, hopefully, before there is any neurological dysfunction.
The hazards of surgery are related to the pre-operative neurological state and the anatomic abnormality. Any infant that already has some element of bladder dysfunction is more vulnerable to having additional problems post-operatively. Children that already have weakness of an extremity or deformity of one or both feet are also at greater risk inasmuch as the neural structures are already fragile and compromised. Conversely, a child who is asymptomatic is at very low risk for being injured by the surgery irrespective of the complexity of the underlying anomaly. An occasional infant has only a short filum terminale (a fibrous band extending from the bottom of the spinal cord to the bottom of the spinal canal) associated with a neurocutaneous signature with no intradural lipoma. This is the simplest of the anatomic abnormalities, and it is only necessary to divide the filum to release the tether. In these cases, the hazard of surgery is more related to infection and anesthesia than any untoward occurrence from surgery. Most cutaneous signatures are anatomically more complex and are associated with an underlying lipoma that extends from the subcutaneous tissues through the bifid spine, through the coverings of the spinal cord and into the fibrous strand extending from the bottom of the spinal cord to the bottom of the spine (the filum). In many cases, the lipoma extends into the spinal cord (an intradural lipoma or lipomyelomeningocele), and in these cases, functioning nerve roots may actually be egressing through the fatty tissue. This is the most complex of the abnormalities, and it is one of the only operations in neurosurgery for which the laser is an indispensable tool. This is because there is a high water content in fat that the laser vaporizes, essentially "melting" the lipoma and making it possible to remove the great bulk of it without injury to adjacent neural structures. In experienced hands, the hazard of surgery is small irrespective of the complexity of the abnormality. The greatest hazard is always to bladder function or, conceivably, to injure a single peripheral nerve to one extremity. However, in the collective experience of pediatric neurosurgeons, the overwhelming likelihood is that there will be no permanent injury from surgery and that the small hazards are far outweighed by the greater hazard of doing nothing.
There Are Two Cutaneous Signatures That May Have Additional Significance
A sinus that is inferior to the lower third of the tailbone of the spine (the sacrum) or over its tip, is, in reality, a pilonidal sinus tract with no neurological importance. These are best treated by a pediatric surgeon in terms of any decision-making vis-à-vis removal or observation. When the identical sinus tract is over the upper two-thirds of the tail bone or at its junction with the lower spine, there is a strong likelihood that the tract is, indeed, passing anteriorly and superiorly into the spinal canal and through the spinal cord's coverings. In these cases, an MRI scan may reveal a tethered spinal cord associated with a short filum or a lipoma or may, in fact, be normal and have no evidence of spinal cord tether. Nevertheless, it is this type of fistula (a passageway lined by skin tissue) that may, in fact, be a conduit for bacteria to pass from the skin's surface into the spinal fluid and cause meningitis. For this reason, all sinus tracts in this location should be excised whether or not there is an associated radiologic abnormality because they may be difficult to visualize in the absence of a tether or associated congenital tumor.
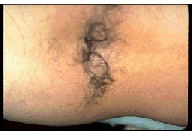
A hairy patch overlying the spine in any area is almost always associated with an underlying splitting of the spinal cord by a band of fibrous tissue or bone (a diastematomyelia). Typically, there is also a short filum and, as a result of both anomalies, a tethered cord. From a surgical perspective, it is only necessary to remove the bony or fibrous band and to divide the filum to treat the entire problem. Little hazard is associated with this, and the prognosis is excellent.
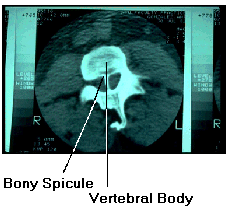
Shown here is a CAT scan of the spine showing a bony spicule dividing the spinal cord. In some cases, the spinal cord can also be divided by a fibrous band that does not contain any bone. ((Photo Needed))
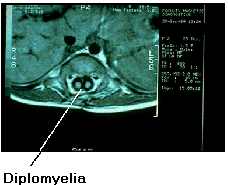
Shown here is an MRI scan of a spinal cord divided by a fibrous band. This condition is termed diastematomyelia (a doubling of the spinal cord in association with either a bony or a fibrous band through the division) and the doubled cord a diplomyelia (diplo = double, myelia = spinal cord). ((Photo Needed))